The danger of germ droplets in dry air!
Water aerosols are the smallest floating particles that contain germs and microorganisms. They enter the air via the respiratory tract when somebody sneezes or coughs and can transmit pathogens such as flu viruses to other people.
The ambient humidity plays a decisive role in germs’ capacity to survive and in the floating behavior of the tiniest aerosol particles. But what exactly is the reason for this?
Germs love dry air
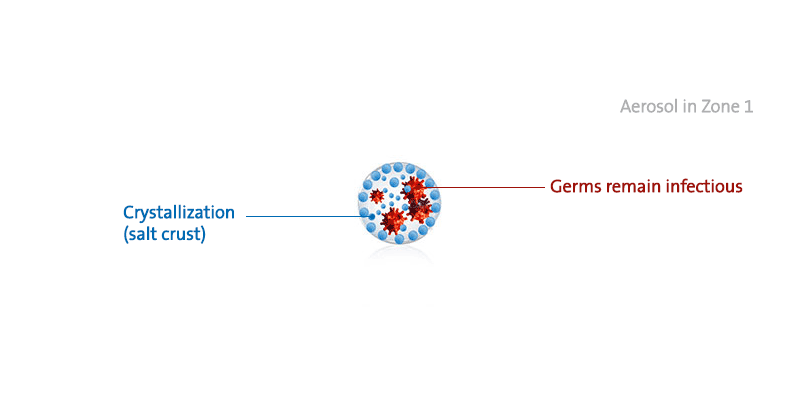
Dry indoor air with a relative humidity proportion of under 40% causes tiny droplets that are loaded with flu or cold viruses to dry up. This preserves pathogens and keeps them infectious for a very long time.
Moist air kills off viruses
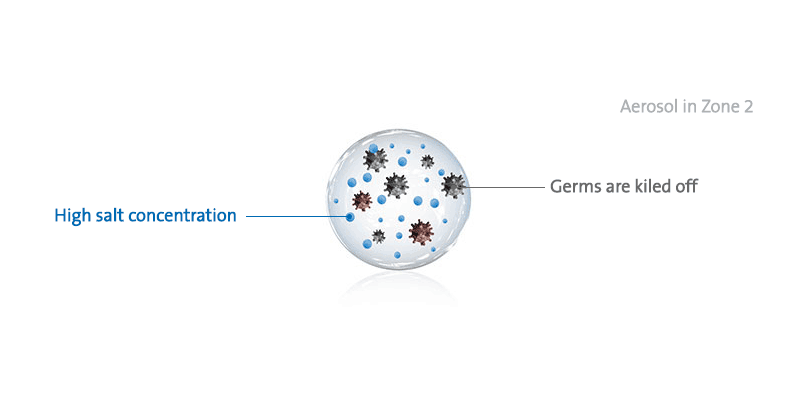
In the optimum range of 40 to 60% relative humidity, aerosols shrink only to such an extent that the salt concentration in the aerosol core increases to the point where the germs and microorganisms it contains are killed off.
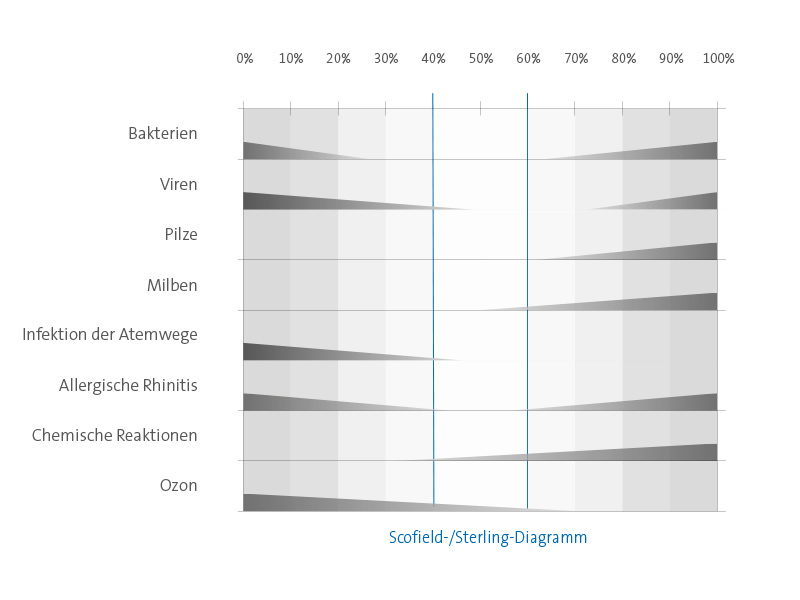
This is also shown in the following contamination diagram according to Scofield/Sterling. Contamination by viruses, germs, fungi or bacteria is the lowest in the range between 40 and 60%. The risk of catching flu and cold viruses is minimal here.
Incapacitation or preservation
The relationship between indoor humidity and microbes by Dr. Walter Hugentobler
Many hygienists, epidemiologists and construction experts still assume that the lowest possible humidity prevents the growth and propagation of bacteria and fungi and contributes to the prevention of diseases.
This view is not correct. Dr. Walter Hugentobler gives an insight into how indoor humidity in buildings affects microbes.
read more
The basic misunderstanding is that “humidity” and “material humidity” are intuitively linked in many people’s minds and wrongly perceived as synonymous. Neither fungi nor bacteria can cover their water requirements from the humidity. They depend on liquid water on non-porous surfaces (condensation water), in porous materials such as gypsum, wallpaper and wood as well as in wet areas (drinking water and sewage systems).
Therefore, the most efficient and healthy way to minimize the water supply to the microbes is not to reduce the indoor humidity, but to improve the insulation of the building shell. As long as the surface temperature does not fall below the critical value (corresponding to 80% equilibrium humidity), no microbial growth can occur. Nevertheless, unsuccessful attempts have been made to prevent the formation of mold through deep indoor humidity for decades. The victims here are the building users, or more specifically, their respiratory tract.
The mucous membranes of the respiratory tract, the eyes and the skin compete with the air for the small amount of water that is still present at low humidity. Since the respiratory tract must condition the dry breathing air to 100% moisture on its way into the alveoli, they dry out. People become susceptible to infections, and the microbes benefit from the ideal conditions for air transmission, as explained below.
Air transfer of microbes
It has been scientifically proven for over 50 years that the air transfer of microbes is promoted by low humidity (and low room temperatures). It has been proven that pathogens for respiratory tract infections (bacteria, flu and cold viruses), but also pathogens of winter diarrhea (rota and noroviruses) as well as fungal spores and fungal fragments can enter the respiratory tract more easily and in larger numbers in dry air. Therefore, reducing humidity to protect against moisture has the side effect of increasing the risk of exposure, not only to mold fungi.
Most microbes know various transmission pathways and preferably choose the one for which the conditions are most favorable at the respective point in time. In heated indoor air, this route is often through the air. Aerogenic transmission via microscopically small droplets, called aerosols, is highly efficient and transport routes are difficult to track. The agent and target of contamination do not have to be temporally or physically closely connected.
A microbe can remain inactive on a surface for days before it reaches its infection target, the humid respiratory tract, via room convection, for example. Research results from several clinical studies with various groups of people show the preventive effectiveness of air humidification during the heating season: Respiratory infections were reduced by 20% in adults and by 50% in children. The number of sick days in the winter fell by 20%.
Physical-biological background
The survival time of airborne flu viruses and other microbes depends on the humidity. While they survive for hours in very high humidity, at a humidity between 40 and 60% they are inactivated within minutes. If the humidity drops below 40%, the viruses and microbes also survive for hours, presumably even considerably longer. They are literally preserved in the dried out droplets. Aerosol physics provides the physical-biological background of this observation: The release of water until the thermodynamic equilibrium state is reached leads to multiple supersaturation of the dissolved and suspended substances at around 50% relative humidity.
This supersaturated solution in the aerosol droplets deactivates the microbes within a few minutes. If the indoor humidity is below a limit value of 40 to 45%, the substances dry out and crystallize within seconds.
The microbes are trapped in the dried aerosols without being deactivated. The cell membranes remain intact and the microbes maintain their ability to cause infection. After renewed hydrogenation, for example after inhalation into a humid respiratory tract, the microbes are released again and can trigger a new infection.
Therefore, the most efficient and healthy way to minimize the water supply to the microbes is not to reduce the indoor humidity, but to improve the insulation of the building shell. As long as the surface temperature does not fall below the critical value (corresponding to 80% equilibrium humidity), no microbial growth can occur. Nevertheless, unsuccessful attempts have been made to prevent the formation of mold through deep indoor humidity for decades. The victims here are the building users, or more specifically, their respiratory tract.
The mucous membranes of the respiratory tract, the eyes and the skin compete with the air for the small amount of water that is still present at low humidity. Since the respiratory tract must condition the dry breathing air to 100% moisture on its way into the alveoli, they dry out. People become susceptible to infections, and the microbes benefit from the ideal conditions for air transmission, as explained below.
Air transfer of microbes
It has been scientifically proven for over 50 years that the air transfer of microbes is promoted by low humidity (and low room temperatures). It has been proven that pathogens for respiratory tract infections (bacteria, flu and cold viruses), but also pathogens of winter diarrhea (rota and noroviruses) as well as fungal spores and fungal fragments can enter the respiratory tract more easily and in larger numbers in dry air. Therefore, reducing humidity to protect against moisture has the side effect of increasing the risk of exposure, not only to mold fungi.
Most microbes know various transmission pathways and preferably choose the one for which the conditions are most favorable at the respective point in time. In heated indoor air, this route is often through the air. Aerogenic transmission via microscopically small droplets, called aerosols, is highly efficient and transport routes are difficult to track. The agent and target of contamination do not have to be temporally or physically closely connected.
A microbe can remain inactive on a surface for days before it reaches its infection target, the humid respiratory tract, via room convection, for example. Research results from several clinical studies with various groups of people show the preventive effectiveness of air humidification during the heating season: Respiratory infections were reduced by 20% in adults and by 50% in children. The number of sick days in the winter fell by 20%.
Physical-biological background
The survival time of airborne flu viruses and other microbes depends on the humidity. While they survive for hours in very high humidity, at a humidity between 40 and 60% they are inactivated within minutes. If the humidity drops below 40%, the viruses and microbes also survive for hours, presumably even considerably longer. They are literally preserved in the dried out droplets. Aerosol physics provides the physical-biological background of this observation: The release of water until the thermodynamic equilibrium state is reached leads to multiple supersaturation of the dissolved and suspended substances at around 50% relative humidity.
This supersaturated solution in the aerosol droplets deactivates the microbes within a few minutes. If the indoor humidity is below a limit value of 40 to 45%, the substances dry out and crystallize within seconds.
The microbes are trapped in the dried aerosols without being deactivated. The cell membranes remain intact and the microbes maintain their ability to cause infection. After renewed hydrogenation, for example after inhalation into a humid respiratory tract, the microbes are released again and can trigger a new infection.
The load is lowest in the range from 40 to 60%!
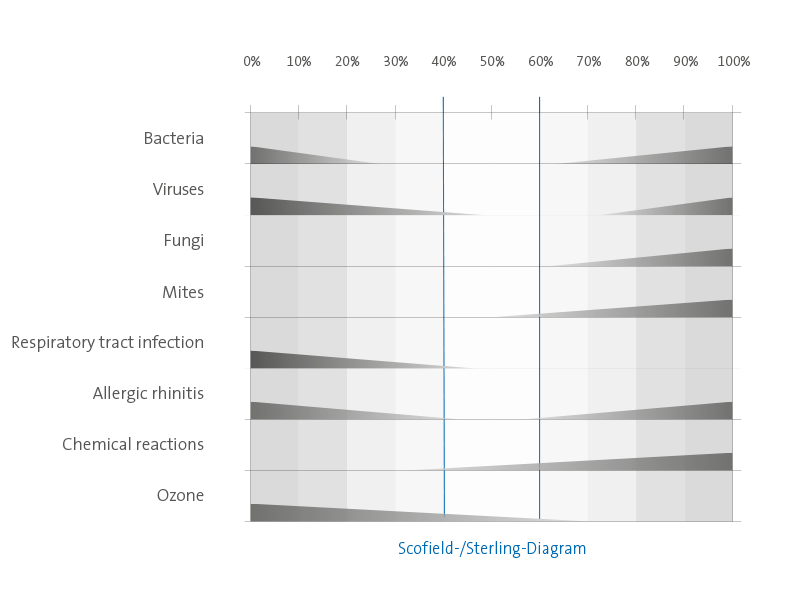
A relative air humidity of 40-60% is optimal for the human body. This range is very unfavourable for germs,
fungi and bacteria, so that the air contains hardly any pollution for humans.
The risk of contracting flu and cold viruses is minimal here.